When yellow tells a story
There are few things as striking in medicine as jaundice. A patient walks in, and before they’ve even said “hello,” their skin and eyes have told you something is wrong.
Jaundice isn’t a diagnosis, it’s a flag. A bright yellow one. Something in the delicate pathway of bilirubin production, metabolism, or excretion has gone sideways.
Your job? Follow the yellow brick road… all the way back to the source.
A quick detour: Bilirubin’s origin story
Every day, your body breaks down old red blood cells. The haem from haemoglobin becomes bilirubin, a pigment that starts off unconjugated (water-insoluble, albumin-bound, and rather antisocial).
The liver then:
- Takes it up
- Conjugates it (thanks to UGT, uridine diphosphate-glucuronyl transferase… try saying that fast)
- Excretes it into bile → bowel → out of the body
Any disruption along this journey, production, conjugation, or excretion, and bilirubin builds up in the blood. Hello, jaundice.
The Three Kingdoms of Jaundice
For exams and sanity-preserving clinical logic, jaundice falls into three main categories:
| Type | Problem | Typical Causes | Clue(s) |
| Pre-hepatic | Too much bilirubin being made | Haemolysis, massive hematoma breakdown | Dark urine absent, ↑ unconjugated bilirubin |
| Hepatic | Liver unable to process bilirubin | Hepatitis, cirrhosis, drugs, sepsis | Mixed pattern LFTs, tender hepatomegaly |
| Post-hepatic (obstructive) | Bilirubin can’t leave | Gallstones, pancreatic cancer, cholangitis | Pale stools, dark urine, pruritus, ↑ ALP & GGT |
If the patient is itching like mad, think obstructive jaundice ⇒ bile salts accumulating in the skin.
LFTs: your biochemical map
A very quick cheat sheet:
- ALT/AST high → liver cell injury
- ALP + GGT high → biliary obstruction
- Bilirubin up alone? → early disease or haemolysis
- Albumin / INR deranged? → failing synthetic function (worry)
And yes, you can impress a consultant by muttering something like:
“This looks like a cholestatic pattern with impaired excretion.”
The Eyes Have It, Clinical Clues
Before technology dazzles you, never forget inspection:
Scleral icterus
Jaundiced skin
Scratch marks (pruritus!)
Spider naevi, ascites → chronic liver disease
Courvoisier’s sign — palpable, non-tender gallbladder → malignancy red flag
Fever + jaundice + RUQ pain → Charcot’s Triad → think ascending cholangitis
Examiners love those patterns.
Tests that will save your surgical career
Start simple:
Blood tests
- LFTs, FBC, Coagulation profile, U&Es
- Viral hepatitis screen
- Hemolysis workup if needed (LDH ↑, haptoglobin ↓)
Imaging
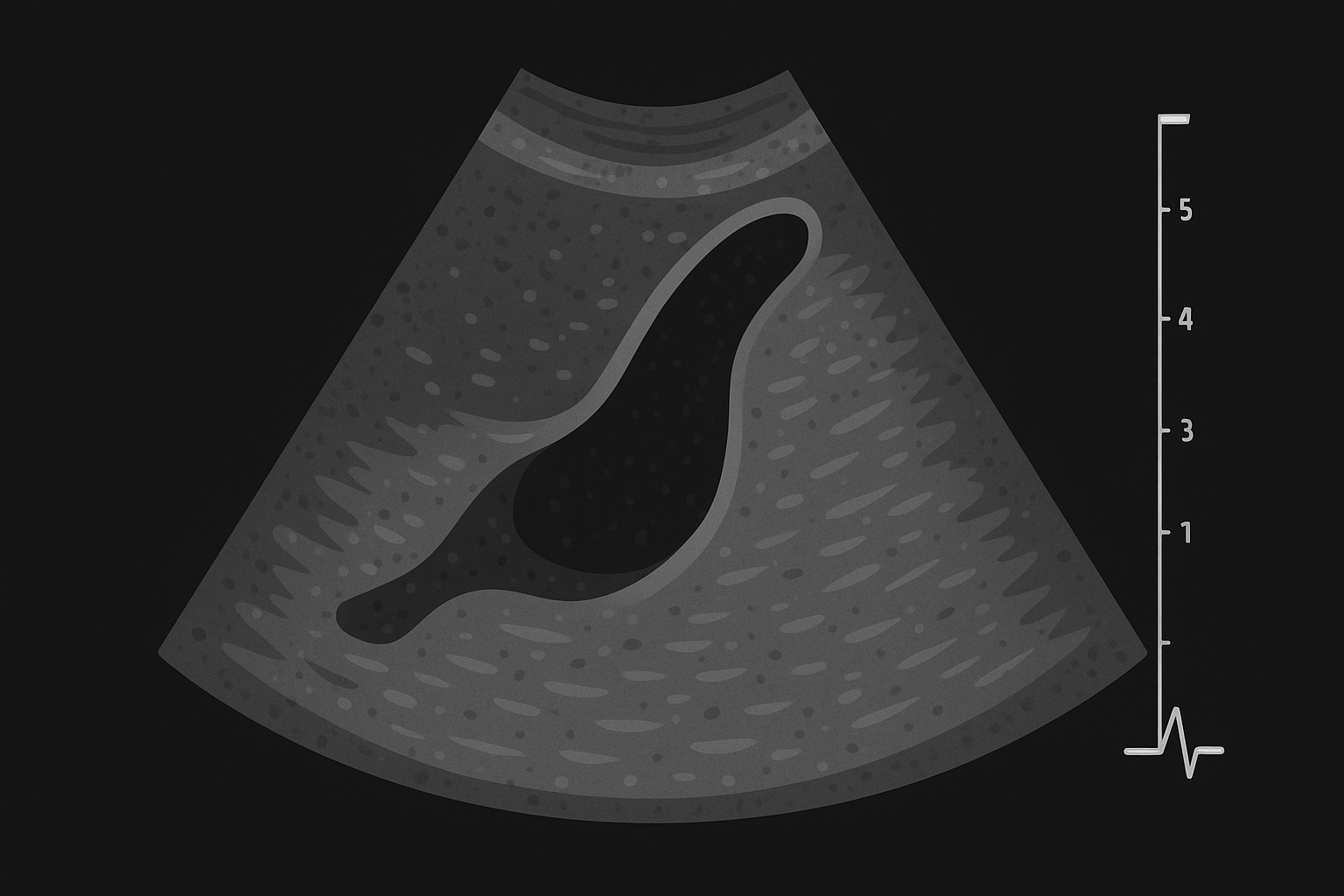
- Ultrasound first → ducts dilated? gallstones?
- MRCP if obstruction suspected
- CT if malignancy suspected
- ERCP when you’re ready to treat the obstruction, not just admire it
And what about newborns?
Ah yes, the tiny yellow humans. Physiological jaundice is common due to immature UGT. But jaundice in the first 24 hours? That’s never normal → think haemolysis or infection.
Treatment, follow the cause
There’s no one-size-fits-all approach:
- Gallstones blocking ducts? → ERCP + cholecystectomy
- Cholangitis? → urgent antibiotics + biliary drainage
- Pancreatic cancer? → stenting, surgical oncology input
- Hepatitis? → supportive + specific therapy
- Hemolysis? → treat underlying cause
Always manage coagulopathy (vitamin K deficiency in cholestasis is common).
A final pearl
If your patient is jaundiced, itchy, and has pale stools + dark urine, the liver is processing bilirubin fine, it’s just trapped. That’s obstructive, until proven otherwise.
And if they look yellow but their urine is normal, think pre-hepatic/haemolysis.
Those two rules alone will get you through half the OSCE stations in existence.
Wrap-up
Jaundice is like a crime scene. The pigment (bilirubin) is the clue, the labs help build the case, and the imaging reveals the suspect. Don’t rush to treat the yellow, find the why.
Because when the body paints itself sunflower yellow, it’s rarely being cheerful about it.