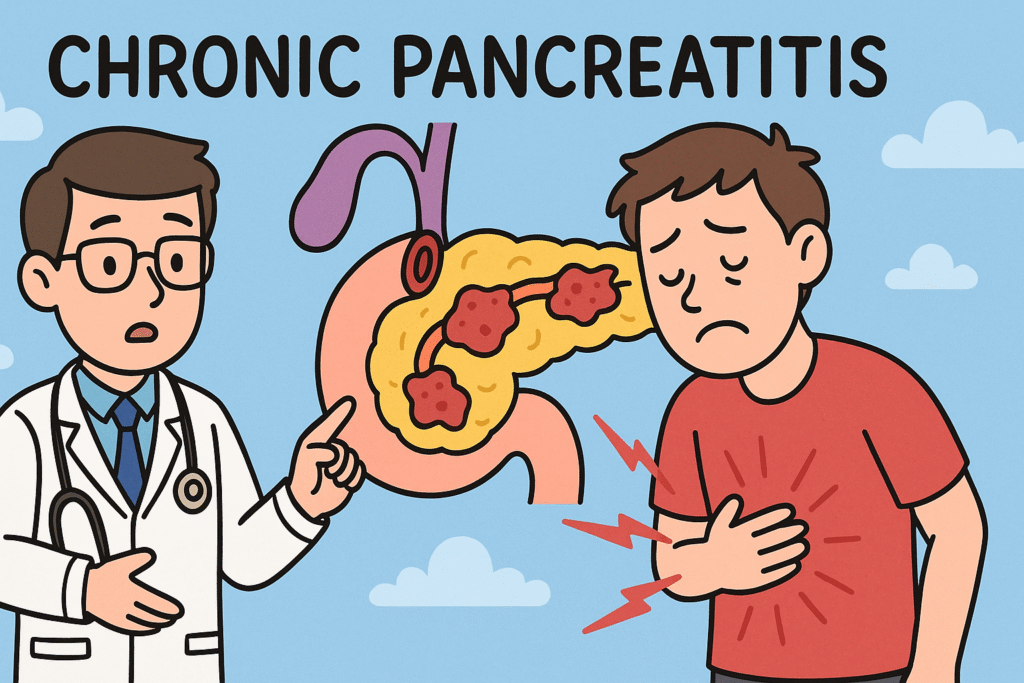
A smouldering rebellion
If acute pancreatitis is an explosion, then chronic pancreatitis is the slow, relentless fire that follows.
The pancreas, once inflamed, never fully forgives. It heals, yes, but with scars instead of cells. Those scars tighten, calcify, and suffocate what’s left of the once-proud enzyme factory.
Over time, this ongoing inflammation and fibrosis strip the pancreas of its two great powers: digestion and endocrine control. What begins as pain after a few drinks ends as malnutrition, diabetes, and a pancreas that’s more rock than organ.
The chronic story, from insult to atrophy
The pathophysiology is tragic in its simplicity. Repeated episodes of pancreatic injury, most often due to alcohol, trigger cycles of inflammation, healing, and scarring. With each round, ducts narrow, pressure rises, and tissue dies.
The acinar cells that once made enzymes disappear, replaced by fibrous tissue and calcium deposits. Eventually, even the islets of Langerhans surrender, leading to pancreatogenic diabetes (Type 3c diabetes, if you want to impress in exams).
The process takes years, but its effects are permanent. Once chronic pancreatitis sets in, the pancreas will never return to its pristine state.
Causes: the usual suspects, plus a few rarities
Like its acute cousin, chronic pancreatitis has two dominant villains: alcohol and genetic predisposition. But its causes are broader and subtler.
| Cause | Mechanism / Notes |
| Alcohol | Chronic toxic injury, ductal obstruction, and oxidative stress. The single most common cause in adults. |
| Genetic | Mutations in PRSS1, SPINK1, CFTR, cause premature enzyme activation and ductal dysfunction. |
| Obstructive | Tumours, strictures, or congenital anomalies (e.g. pancreas divisum). |
| Autoimmune | Immune-mediated fibrosis; part of the IgG4-related disease spectrum. |
| Idiopathic | No identifiable cause — more common in younger and tropical populations. |
In the tropics, an enigmatic entity called tropical calcific pancreatitis afflicts young adults, often linked to malnutrition and cassava toxins. It’s a cruel disease of poverty: patients waste away before their time; their pancreas turned to stone.
The pain that won’t quit
The hallmark of chronic pancreatitis is pain, deep, gnawing, and exhausting.
It often sits in the epigastrium, radiates to the back, and worsens after meals or alcohol. At first, it comes in bouts; later, it becomes relentless. The pain reflects ductal obstruction and neural inflammation rather than enzyme leakage, which is why enzyme levels (amylase, lipase) are often normal.
As the disease advances, some patients note a bittersweet reprieve: the pain fades. But it’s not mercy, it’s atrophy. The pancreas has burned itself out, leaving nothing left to inflame.
The slow collapse of function
Exocrine failure comes first. With dwindling enzyme output, fat digestion falters. Patients develop steatorrhoea, greasy, foul-smelling stools that float, leaving an oily film on the toilet water. Weight loss follows, along with vitamin deficiencies (especially A, D, E, and K).
Then comes endocrine failure, as the islets die. The result is diabetes mellitus, but with a twist: unlike Type 1 or Type 2, there’s little glucagon reserve, making hypoglycaemia a constant threat.
Diagnosis: sometimes the hardest pancreas to prove
Unlike acute pancreatitis, chronic pancreatitis doesn’t shout, it whispers.
Blood tests may be normal. Enzymes often aren’t elevated. The real evidence lies in imaging and function tests.
- CT or MRI: show ductal dilatation, gland atrophy, and the pathognomonic pancreatic calcifications.
- MRCP: gives exquisite ductal detail without the risk of ERCP-induced injury.
- Endoscopic Ultrasound (EUS): detects early parenchymal and ductal changes before calcifications appear.
- Fecal elastase test: a simple, non-invasive marker of exocrine insufficiency; low levels confirm functional loss.
In autoimmune pancreatitis, serum IgG4 levels are often raised, and imaging may show a “sausage-shaped” gland with a rim of halo enhancement, classic exam bait.
Management: playing the long game
There’s no cure for chronic pancreatitis. The goal is to control pain, replace lost function, and prevent complications.
1. Lifestyle and cause control
- Absolute alcohol abstinence, the first, second, and third rule.
- Stop smoking; it accelerates fibrosis.
- High-calorie, low-fat meals in small, frequent portions.
2. Pain management
Start simple, climb carefully. Paracetamol and NSAIDs may suffice early, but many require opioids.
Enzyme supplements sometimes reduce pain by suppressing endogenous pancreatic stimulation.
When medical therapy fails, endoscopic decompression (stone removal, duct stenting) or surgical drainage (e.g., Puestow or Frey procedure) can relieve ductal hypertension.
3. Enzyme replacement therapy
Pancreatic enzyme supplements, usually enteric-coated preparations of lipase, amylase, and protease, are essential. They should be taken with meals, not before or after.
Add fat-soluble vitamin supplements and proton pump inhibitors to optimise absorption.
4. Diabetes management
Pancreatogenic diabetes is brittle and unpredictable. Insulin is often required, and hypoglycaemia vigilance is key.
5. Treat complications
Chronic pancreatitis breeds trouble:
- Pseudocysts: fluid collections that can compress ducts or vessels.
- Biliary strictures: from scarring near the pancreatic head.
- Splenic vein thrombosis: leading to gastric varices.
- Pancreatic cancer: the long-term spectre; chronic inflammation is a carcinogenic soil.
Any patient with new-onset jaundice, back pain, or weight loss deserves urgent evaluation for malignancy.
A word on autoimmune pancreatitis
Autoimmune pancreatitis deserves its own brief spotlight. It often masquerades as pancreatic cancer, presenting with painless jaundice and a diffusely enlarged gland.
The key is its steroid responsiveness, give prednisolone, and the gland shrinks dramatically, almost theatrically. Recognising it spares patients a needless Whipple procedure.
Life after diagnosis: a marathon, not a sprint
Patients with chronic pancreatitis live with a constant companion, pain, dietary restriction, and fatigue. Depression, malnutrition, and social isolation are common.
A multidisciplinary approach is essential: gastroenterologists, surgeons, dietitians, pain specialists, and psychologists all have roles to play.
For clinicians, it’s a humbling disease. You can’t fix it; you can only steady the patient for the long road ahead. For patients, it’s a lifelong lesson in restraint and resilience.
The closing line
Acute pancreatitis screams; chronic pancreatitis sighs. One kills quickly, the other slowly erodes.
Both remind us that the pancreas, that modest retroperitoneal gland, holds more power than its size suggests.
“You can provoke it once and escape, but torment it long enough, and it will burn you quietly from within.”