The great escape…
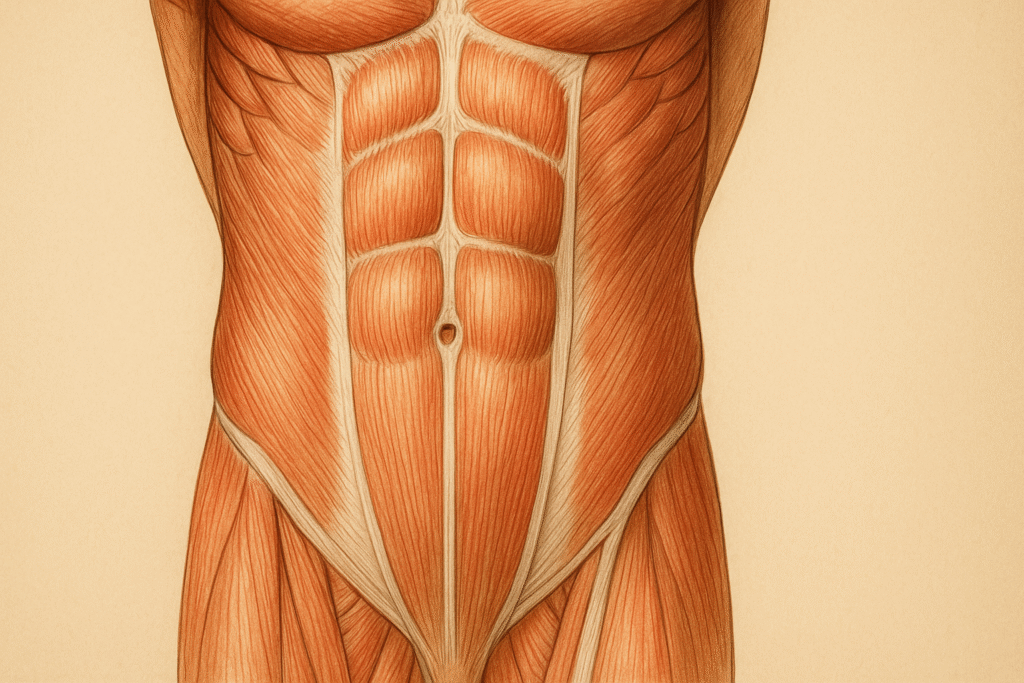
The abdominal wall is a masterpiece of engineering, layers of muscle, fascia, and peritoneum that hold back the constant pressure of life: breathing, coughing, eating, lifting, laughing, and occasionally regretting.
But even the best architecture has weak points.
And when the inner contents, usually omentum or bowel, find one, they make a break for it.
That, dear reader, is a hernia: the great escape of the abdominal contents through a weak spot in the wall that was never designed to let them out.
Definition, in plain English
A hernia is a protrusion of a viscus (or part of it) through a defect in the wall of the cavity that normally contains it.
In this case, we’re talking about the anterior abdominal wall, meaning hernias that appear on the front of the abdomen, from the xiphoid to the groin, from the midline to the flank.
They’re common, often harmless at first, but occasionally lethal if strangulation occurs.
Anatomy of a misbehaviour
Every hernia has three parts, think of it as a rebellious story with structure:
- The neck: the defect or weakness through which contents emerge.
- The sac: a pouch of peritoneum that protrudes through the defect.
- The contents: omentum (fat), bowel, or sometimes even stomach or bladder, depending on location and creativity.
The wall’s weak points correspond neatly to where muscles, fascia, or vessels leave gaps, nature’s oversight, and the surgeon’s playground.
The cast of characters: types of anterior abdominal wall hernias
Let’s meet the usual suspects, from top to bottom.
| Type | Location | Notes |
| Epigastric hernia | Between xiphoid and umbilicus, in the midline (linea alba) | Small defect through which preperitoneal fat escapes. Common in fit young men. “Painful lump above the belly button.” |
| Umbilical hernia | At the umbilicus | Congenital in infants (usually closes spontaneously). In adults, often from obesity, pregnancy, or ascites. |
| Paraumbilical hernia | Adjacent to the umbilicus (not through it) | Common in obese multiparous women; can enlarge to alarming proportions. Prone to strangulation. |
| Incisional hernia | At the site of a previous surgical scar | Iatrogenic weakness; up to 15% of laparotomy wounds. The revenge of poor closure, infection, or tension. |
| Spigelian hernia | Along the semilunar line (lateral edge of rectus muscle, below umbilicus) | Sneaky and hard to spot; often between muscle layers; requires imaging to confirm. |
| Richter’s hernia | Any site (especially femoral) | Only part of bowel wall herniates, so no obstruction; but strangulation risk is sky-high. |
| Lumbar or flank hernias | Posterolateral abdominal wall | Rare and usually post-traumatic or post-surgical. |
If you can remember the names, the rest is anatomy and pattern recognition.
Risk factors: the pressure equation
Hernias are born when two forces meet: increased intra-abdominal pressure and weak abdominal walls.
Pressure-raisers:
- Chronic cough
- Constipation
- Heavy lifting
- Pregnancy
- Obesity
- Ascites
- Prostatic obstruction
Wall-weakeners:
- Age
- Malnutrition
- Collagen disorders
- Surgical wounds
- Steroid therapy
The balance between strength and strain determines your fate.
The patient’s story
Most hernias start as a small, soft swelling that appears on straining and disappears on lying down. The patient will say things like:
“It pops out when I cough, doctor.”
“I can push it back in.”
“It doesn’t hurt, unless I lift something.”
But beware the change in tone, when the hernia becomes painful, irreducible, or tender, the game changes. That’s when incarceration or strangulation have entered the scene.
Examination: the gentle art of hernia hunting
Inspect, palpate, and think.
Inspection:
- Expose the abdomen fully.
- Look for scars (especially midline or transverse laparotomy scars).
- Observe for visible bulges, asymmetry, or movement with coughing.
Palpation:
- Feel the lump, soft or firm? Reducible or fixed? Tender?
- Ask the patient to cough, feel for an expansile cough impulse, the hallmark of a true hernia.
- Try to reduce it gently; note if contents slip back easily.
- Examine for complications, irreducibility, tenderness, redness, warmth.
If it’s an incisional hernia, measure the defect and check the integrity of the surrounding muscle.
If you’re unsure, ultrasound or CT can confirm, especially for Spigelian or recurrent hernias.
Complications, when a bulge becomes a battle
- Incarceration: contents get trapped; hernia no longer reducible.
- Strangulation: blood supply to trapped contents is cut off, severe pain, tenderness, systemic toxicity, bowel necrosis.
- Obstruction: if bowel is trapped, patient develops vomiting, distension, and constipation.
- Skin ulceration or rupture, in massive, neglected cases.
The progression from “painless lump” to “life-threatening emergency” can take hours.
Management: from watchful waiting to mesh masterpieces
1. Conservative (in selected cases)
- Small, asymptomatic hernias in unfit or elderly patients can be managed with observation and abdominal support garments.
- But every hernia deserves respect, they never heal themselves.
2. Surgical repair (the definitive cure)
Modern hernia surgery is about tension-free reinforcement.
The days of simple suture repair are largely gone; mesh is now the star.
- Open repair: straightforward, especially for small or incisional hernias.
- Laparoscopic repair: ideal for recurrent or bilateral hernias; smaller scars, faster recovery.
- Component separation or complex reconstruction: for giant or multiple incisional hernias.
Principles:
- Return contents to the abdomen.
- Excise or reduce the sac.
- Strengthen the defect with mesh.
And yes, optimize before operating, control cough, lose weight, correct nutrition, stop smoking. The wall will thank you.
Special mention: incisional hernias, the surgeon’s hangover
An incisional hernia is the scar’s way of reminding you that closure is an art, not a reflex.
Risk factors include infection, obesity, poor technique, excessive tension, or early strain.
These hernias often enlarge progressively and may contain loops of bowel or omentum. Repair can be challenging, especially when tissue quality is poor.
Laparoscopic or on lay mesh repairs have transformed outcomes, but recurrence remains a risk if patient factors aren’t optimised.
Prevention: the forgotten cure
The best hernia repair is the one you never have to do.
So:
- Use meticulous surgical technique.
- Close laparotomy wounds with continuous, mass closure, adequate bites, and appropriate suture.
- Treat chronic cough, constipation, or ascites early.
- Encourage weight loss and core strengthening.
Surgeons may love fixing hernias, but prevention is the quiet triumph.
Clinical pearls
- Any lump on the abdominal wall that coughs, reduces, and returns is a hernia until proven otherwise.
- Strangulated hernia = emergency surgery.
- Spigelian hernia often hides between muscle layers, think of it in unexplained abdominal pain.
- Incisional hernia is the most common late complication of laparotomy.
- Never attempt to reduce a tender, irreducible lump, you may push necrotic bowel into the peritoneum.
Anterior abdominal wall hernias are the body’s polite reminder that pressure always finds a way out.
They begin as curiosities, a bulge, a nuisance, a conversation piece, and end, if neglected, as surgical emergencies.
Every hernia tells a story of structure under strain. Your job is to read it early, respect it always, and repair it properly.
Because when the gut decides to step outside, it’s best to show it the way back, before it burns the house down.