Because sometimes, preservation isn’t an option, and hesitating costs lives.
The Reality in the Trauma Bay
The spleen doesn’t leak; it gushes. When it tears, the blood is everywhere before you’ve even got both gloves on. You’ll want to save it if you can, immune function matters, but trauma doesn’t care about immunology lectures.
Sometimes the spleen makes the decision for you: it’s pulped, devascularised, or simply refusing to stop bleeding despite packing and pressure. That’s when you take it out, fast, controlled, and without adding new problems.
So, here’s how I do a trauma splenectomy when the clock is eating the patient alive.
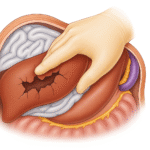
Step 1 – Exposure: Make Space Before You Bleed Into It
- Midline laparotomy (don’t waste time with subcostal incisions in trauma).
- Scoop clots. Pack quadrants. especially the left upper quadrant.
- Lift the diaphragm-facing packs last, you want the spleen to be the final reveal, not an explosion of blood.
If the patient’s crashing:
- Pack around the spleen immediately → hilar control on standby → blood to hand.
- Don’t spend a minute searching for elegance. Control the battlefield first.
Step 2 – Control the Hilum Early
Blood loss is fastest at the hilum, so this is the prize.
Key options:
- Direct vascular stapler across the hilum (my preference in unstable patients).
- Individual ligation of splenic artery and vein if the field is clean and perfusion is stable.
- If the spleen is shredded and visibility is hell:
- Find pancreas tail first → work above it, not through it.
Golden rule:
Control inflow/outflow early, not after the spleen is hanging by a thread.
Step 3 – Mobilisation: Free the Spleen Without Maiming the Pancreas
Start lateral, move medial:
- Divide splenocolic ligament
- Open phrenicocolic ligament
- Divide splenorenal and splenophrenic ligaments
- Keep the pancreatic tail in your mind’s eye at all times
Gentle retraction, the capsule tears if you look at it wrong.
Danger zone:
The short gastrics.
- Use energy or clips.
- A splash of arterial blood from a posterior gastric branch at the wrong moment will ruin your mood and the anaesthetist’s day.
Step 4 – Remove the Organ
Once the hilar control is secure and ligaments are divided:
- Lift and deliver the spleen into your hand
- Double-check for bleeding from:
Hilar stumps
Pancreatic tail
Short gastrics
Diaphragmatic side tears
If unstable → pack and get out (damage control).
If stable → irrigate, inspect, close more elegantly.
Step 5 – Search for the Sneaky Accessory Spleens
Just when you think you’re done…
Accessory spleens can be anywhere:
- Along splenic vessels
- In the omentum
- Near the pancreas tail
- In the gastrosplenic ligament
If this was trauma + underlying disease (ITP, spherocytosis), finding them is mandatory.
In pure trauma? Still worth a quick look, especially in young patients.
Step 6 – Drain and Protect
- Place a drain if:
- Pancreatic tail was manipulated
- Hilum visibility was poor
- Ongoing oozing exists
- Close without tension
- If you packed → temporary closure and plan for relook
Documentation: number of packs, hilum technique, pancreas check, estimated blood loss.
ICU Handover: The Battle Isn’t Finished
Post-splenectomy concerns:
- Thrombocytosis, watch trends
- OPSI risk (overwhelming post-splenectomy infection)
- Vaccination planning once stable
- Pain control (diaphragmatic irritation hurts like hell)
Coordinate with ICU: warmth, balanced transfusion, electrolytes (calcium), and close watch on drains.
Pearls & Pitfalls (AKA Lessons Paid in Blood)
- The spleen tears again the moment you let go → control hilum first
- Never forget the pancreatic tail is collateral damage waiting to happen
- A stapler is a beautiful thing in a dying patient
- If you can’t see, you don’t dissect; pack, resuscitate, return
- Don’t chase accessory spleens while the MAP is 40
- Leave the OR with physiology trending up, not down
And From the Patient’s Side…
They won’t remember the chaos, the blood, the clamps, the urgency in your voice.
They’ll just wake up missing an organ they never thought about once in their life.
For them, splenectomy isn’t damage control, it’s survival.
A second chance bought with your decisiveness, your steady hands, and the discipline to act when waiting would cost them everything.