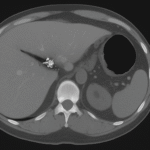
The unassuming culprit
It’s small, pear-shaped, and tucked quietly beneath the liver, yet it’s responsible for an astonishing number of admissions, operations, and late-night calls to surgical registrars. The gallbladder may look innocent on diagrams, but when it decides to make stones, chaos follows.
Gallstones, or cholelithiasis, if you want to impress your examiner, are one of the most common digestive disorders. They can cause pain, jaundice, pancreatitis, and, sometimes, no symptoms at all (which is somehow even more irritating).
Let’s unpack this, one thoughtful layer at a time.
The gallbladder: a quick recap
Think of the gallbladder as the bile storage and concentration unit. The liver is constantly making bile, about 500–1000 mL per day, but we don’t need it all the time. So, the gallbladder stores it, concentrating it five- to tenfold, ready to squirt it into the duodenum after a fatty meal (the classic “right upper quadrant fireworks” trigger).
Bile itself is a cocktail of bile salts, cholesterol, phospholipids, and bilirubin, all kept in a delicate balance. Tip that balance, and precipitation happens. Chemistry turns to pathology.
The recipe for stones
There are two broad flavours of gallstones:
- Cholesterol stones, the commonest type (around 80%).
- Formed when bile becomes supersaturated with cholesterol.
- Risk factors follow the famous “5 Fs”: Fair, Female, Forty, Fertile, and Fat.
- Add to that: rapid weight loss, oestrogen therapy, diabetes, and certain ethnic backgrounds (especially Native American).
- Pigment stones, darker, smaller, and less common.
- Black pigment stones: seen in chronic haemolysis (e.g., sickle cell disease, hereditary spherocytosis).
- Brown pigment stones: linked to infection or stasis in the biliary tree, more common in the Far East.
Sometimes, patients manage to grow a mixed stone, because why settle for one pathology when you can have two?
How gallstones cause trouble
Most gallstones live their lives in peaceful obscurity, found incidentally on an ultrasound ordered for “bloating” or “non-specific abdominal discomfort.” But when they move, they make themselves known.
The location of the stone determines the syndrome:
| Location | Result | Key Features |
| Gallbladder lumen | Biliary colic | Episodic right upper quadrant pain, often after fatty meals, radiating to the back or right shoulder; normal labs |
| Cystic duct (obstruction) | Acute cholecystitis | Persistent pain, fever, leucocytosis, positive Murphy’s sign |
| Common bile duct | Choledocholithiasis | Jaundice, dark urine, pale stools, elevated ALP & bilirubin |
| Ampulla of Vater | Gallstone pancreatitis | Epigastric pain radiating to the back, elevated amylase/lipase |
| Gallbladder wall (chronic irritation) | Chronic cholecystitis | Thickened gallbladder, fibrosis, recurrent attacks of pain |
In short, the stone rolls, the duct blocks, pressure builds, inflammation follows, and the patient ends up clutching their right side while you mutter about Murphy’s sign and start ordering an ultrasound.
The pain: clinical poetry in motion
Biliary colic is a misnomer, it’s not colicky at all. It’s a steady, gripping pain in the right upper quadrant or epigastrium, peaking within an hour, often after a heavy meal. The pain may radiate to the right shoulder (via the phrenic nerve, C3–C5 dermatome, exam gold).
When inflammation joins in (acute cholecystitis), the pain becomes more persistent, fever develops, and the Murphy’s sign, cessation of inspiration due to pain on palpation, becomes your diagnostic friend.
Diagnosis: see it to believe it
Ultrasound is the first and best investigation, sensitive, non-invasive, and quick. It’ll show stones as echogenic foci with acoustic shadowing. You might also see a thickened wall or pericholecystic fluid in cholecystitis.
If you suspect a common bile duct stone, add an MRCP (magnetic resonance cholangiopancreatography). If the patient is jaundiced and febrile (Charcot’s triad: pain, fever, jaundice), think ascending cholangitis, a true surgical emergency.
Management: from calm to crisis
Asymptomatic stones? Leave them alone. They’re like quiet tenants, don’t evict unless they cause trouble.
Symptomatic or complicated stones? That’s a different story.
- Acute cholecystitis
- IV fluids, antibiotics, analgesia.
- Early laparoscopic cholecystectomy (within 72 hours if possible).
- Choledocholithiasis
- Endoscopic retrograde cholangiopancreatography (ERCP) to remove the stone, followed by cholecystectomy.
- Gallstone pancreatitis
- Supportive care for pancreatitis first.
- Cholecystectomy during the same admission once stable.
- Chronic cholecystitis
- Elective laparoscopic cholecystectomy.
Laparoscopic surgery is the standard now, quicker recovery, smaller scars, and fewer hernias. But remember, not every abdomen is friendly. Dense adhesions, Mirizzi’s syndrome, or unclear anatomy can push you to convert to open, and that’s okay. Safety first.
A word on complications
Gallstones are mischievous. Left long enough, they can cause:
- Empyema or gangrene of the gallbladder
- Perforation and peritonitis
- Gallstone ileus (a large stone erodes into the duodenum and lodges in the terminal ileum)
- Porcelain gallbladder, which carries a risk of carcinoma
Exam essentials
If you’re revising, here’s the quick-fire list you’ll need to remember:
- Risk factors: Female, Forty, Fertile, Fat
- Pain: Postprandial, right upper quadrant, radiates to shoulder
- Investigations: Ultrasound first, MRCP for ducts
- Complications: Cholecystitis, cholangitis, pancreatitis
- Treatment: Laparoscopic cholecystectomy ± ERCP
And if an examiner asks why the pain radiates to the shoulder, smile and say:
“Because the gallbladder shares sensory innervation with the diaphragm via the phrenic nerve (C3–C5).”
That’s anatomy, physiology, and embryology, all in one sentence.
The takeaway
Gallstones are one of surgery’s great equalizers, everyone from medical students to consultants encounters them. Learn them well. Understand the pathophysiology, not just the buzzwords. Remember that every patient is a bit different, some will have classic textbook signs, others will present like a mystery novel.
And always, always confirm with an ultrasound before you declare “biliary colic” in the middle of the night. Trust me on that one.